HIV testing and status awareness among key populations (A-D)
Export Indicator
This indicator is divided into four sub-indicators:
A. HIV testing among sex workers.
B. HIV testing among men who have sex with men.
C. HIV testing among people who inject drugs.
D. HIV testing among transgender people.
What it measures
Progress providing HIV testing services to members of key populations.
Ensuring that people living with HIV receive the care and treatment required to live healthy, productive lives and reduce the chance of transmitting HIV, requires that they know their HIV status. In many countries, targeting testing and counselling for locations and populations with the highest HIV burden is the most efficient way to reach people living with HIV and ensure that they know their HIV status. This indicator captures the effectiveness of HIV testing interventions in reaching populations at higher risk of HIV infection.
Respondent knows they are living with HIV (answer to Question 3 is “positive”)
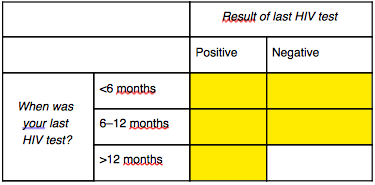
The number of respondents in the yellow boxes is the numerator.
Number of people in key populations who answered question Question 1 (below).
Numerator/denominator
Every two years
A, C: Gender (female, male and transgender).
D: gender (transman, transwoman, other)
A-D: Age (<25 and 25+ years).
If there are subnational data available, please provide the disaggregation by administrative area, city, or site in the space provided. Submit the digital version of any available survey reports using the upload tool.
HIV testing and counselling is the necessary first step to addressing a person’s HIV infection. People living with HIV need to be aware of their HIV status and able to make use of prevention and treatment services for their own health and to prevent transmission of the virus. National programmes aim to have 95% of people who are living with HIV know their HIV status.
HIV-positive respondents may be less willing to accurately report their HIV status than HIV-negative respondents, leading to under-reporting of testing coverage among people living with HIV.
Global HIV Strategic Information Working Group. Biobehavioural survey guidelines for populations at risk for HIV. Geneva: World Health Organization; 2017 (http://www.who.int/hiv/pub/guidelines/biobehavioral-hiv-survey/en/).
Related Indicators
TL.6 Know their status (key population), 2020, WHO Consolidated HIV strategic information guidelines: driving impact through programme monitoring and management (https://www.who.int/publications/i/item/consolidated-hiv-strategic-information-guidelines).