(HRH_CURR) Number of health workers who are working on HIV-related activities and are receiving any type of support from PEPFAR, as well as total spend on these workers
Export Indicator
This indicator measures the number of PEPFAR-supported health workers who contribute to providing HIV services at facility and community sites. It allows us to track our level of support and continuously calibrate it based on impact. It also allows us, over time, to measure the transition from PEPFAR support to host country support.
Many countries experience HRH shortages and/or imbalances by population density (e.g., HRH shortages in rural areas) that are not related to population health needs, including HIV epidemiology. Addressing density and distribution of HRH is important in increasing access to HIV services where they are needed.
In many PEPFAR countries, there are overall shortages of HRH, particularly in rural and remote areas, leading to insufficient numbers of health workers according to internationally recommended levels (2.3 doctors, nurses, midwives/1,000 population). There are also countries where there is large overproduction of health workers, with medical unemployment in urban areas, and at the same time with shortages in rural areas.
Furthermore, different types of health workers receive different types and amounts of support that may vary by geographic location, cadre, workload, and other factors. Understanding the ways in which different cadres are supported is important for mobilizing differential models of service delivery under different circumstances.
Number of health workers at this facility site who are working on HIV-related activities (e.g., prevention, treatment) and are receiving any type of support from PEPFAR, as well as total spend on these workers
N/A
How to calculate annual total:
N/A. Data is reported only once annually at Q4.
Fill out total # of de-duplicated staff entry form first, and then complete the disaggregates. Data should capture health workers for whom PEPFAR provided support in the same reporting period (fiscal year), and who have not been transitioned by the end of the fiscal year. Unfilled positions or vacancies should not be included.
How to collect:
Data on total numbers of positions supported should be tracked by implementing partner’s record-keeping systems, for example, personnel databases, human resources records, and financial records that show salary or stipend payments, including information on non- monetary support to volunteers. Leverage the same records and systems partners already use to report dollar amounts for work plans and financial reporting, to identify PEPFAR support of HRH.
For non-monetary supported personnel, partners should cross-reference expense reports and registers against the cadre types who received the corresponding non-monetary benefits. For example, receipts showing transportation allowances were provided to attend meetings could be cross-referenced with the attendance listed in the minutes for community lay workers.
Facility and community workers are reported by IM, Site ID, facility and community site affiliation, and cadre type. All PEPFAR-supported workers at the facility and community should be reported.
How to document:
- Identify all facility and community sites where you work.
- Identify and count the number of health workers (individuals) you support at each site.
- Group these health workers into their most appropriate, mutually exclusive cadre (doctor, nurse, lay counselor, laboratory cadres, pharmacy cadres, etc.).
- List the total number of workers by each cadre under the “total # of de-duplicated staff by cadre” column. This numerator is entered separately in DATIM, separate from the disaggregates described below.
- List all types of monetary and non-monetary support that were provided to health workers at any of those sites in the current fiscal year (as incentive or compensation for time spent on HIV services at those sites).
- It is possible for one worker to receive more than one type of support. In such cases individual staff person can be listed under more than one type of support. It is possible for the disaggregates to exceed the numerator for each cadre. However, note that the entries under “total # of de-duplicated staff by cadre” column should be the actual number of workers supported by PEPFAR.
- Salary support includes base salary.
- Stipend includes any amount paid that is above the standard base salary, allowances, and financial benefits such as health insurance, social security benefits, fringe benefits, etc. For example, a health worker that works out of standard business hours such as a weekend, and PEPFAR pays for weekend hours only.
- Assign those types of support to the health workers identified on your site lists and then create a matrix of supported health workers by cadre and support type.
- Non-monetary support should be reported even if you provide only non-monetary support, with no salary or stipend.
- Above-site support may include Ministry of Health or other government staff who work at the district or provincial level, or at the national level, including Ministry of Health office, National Reference Laboratories, or at national research centers not otherwise providing HIV services directly to beneficiaries.
How to review for data quality:
Sites reporting on HRH_CURR should be reporting DSD results for the indicators that the HRH are supporting.
HRH_STAFF_NAT should be greater than or equal to HRH_CURR at each individual site (facility-level only) where these data are reported. HRH_STAFF_NAT includes all staff at PEPFAR-supported sites (i.e., staff that are both PEPFAR-supported AND non-PEPFAR supported).
The total number of workers reported under the column “total # of de-duplicated staff by cadre” cannot be higher than the sum of disaggregates. However, it can be lower than the sum of disaggregates.
Reporting level: Facility, Community, and Above-Site
Reporting frequency: Annually
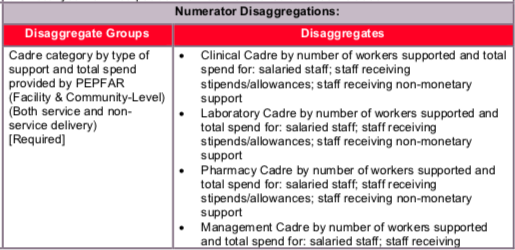
- Clinical workers are those who provide a direct clinical service to clients: Clinical professionals, including doctors, nurses, midwives, clinical officers, medical and nursing assistants, auxiliary nurses, auxiliary midwives, and testing and counseling providers. They should have completed a diploma or certificate program according to a standardized or accredited curriculum and support or substitute for university-trained professionals.
- Laboratory workers are those who conduct laboratory tests, collect blood or samples at a lab, and relay the results to a clinician for diagnostic purposes. This category includes cadres such as laboratorians, lab technicians, phlebotomists, and lab managers.
- Pharmacy workers are those who dispense ARVs at a facility or community center and help with forecasting and supply chain logistics to ensure there are no stock-outs. It includes but not limited to pharmacists, pharmacy assistants, and pharmacy technicians based at a facility.
- Management workers are those who provide support to the site for administrative needs but not directly provide services to clients: Facility administrators, human resource managers, monitoring and evaluation advisors, epidemiologists and other professional staff critical to health service delivery and program support.
- Social service workers are those who have advanced training in social services and provide services directly to clients: Social service workers including social workers, child and youth development workers, social welfare assistants.
- Lay workers are those who have non-clinical training and provide services directly to clients: Health workers who provide important services for the continuum of care within facilities and/or communities. These include but are not limited to adherence support, mother mentors, cough monitors, expert clients, lay counselors, peer educators, community health workers and other community-based cadres.
- Other HCWs: workers who do not fit into any of the categories above (e.g., data capturers, data clerks, security guards, cleaners, etc.).
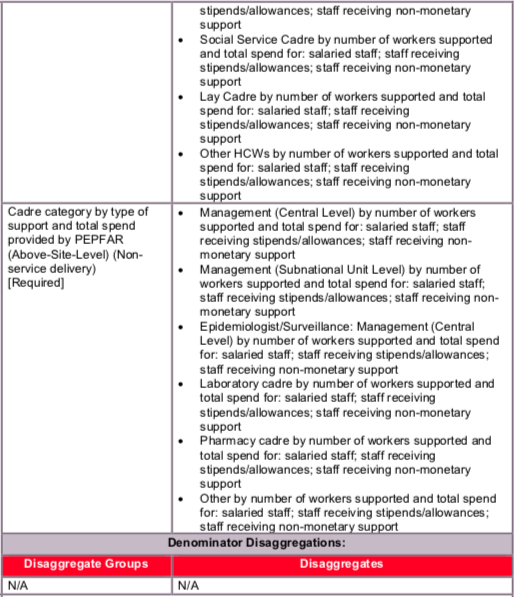
Cadre Category (Above-Site-Level; non-service delivery):
- Management central level are those staff supporting management functions at national level. Examples may be development and implementation of policies, guidelines, quality standards, health or HIV budgeting and financing. The work of these staff has a national scope and affect all (or multiple) districts or regions.
- Management sub-national unit are those staff supporting management functions for one geographic area at the sub-national level. Examples may include district-level health planning and coordination, district-level quality improvement, training or mentoring (e.g., district health office, provincial coordinating authority)
- Laboratory workers are those staff providing monitoring and supportive supervision, and in-service training to facility-based lab workers. These may include laboratory QI specialists, lab accreditation specialists at the PSNU or OU level, and secondments for the lab branch in a Ministry of Health.
- Pharmacy workers are those managing various stages in the supply chain process, including forecasting and logistics above the service delivery level. It includes but not limited to pharmacy managers, staff at a drug warehouse involved in supply chain logistics, pharmacists based at the SNU level, and senior pharmacists/ secondments based at a Ministry of Health.
- Epidemiologist/Surveillance staff are those collecting and/or analyzing HIV epidemiologic data at the above-service delivery area level. This may include making national or district-level estimates of PLHIV or key populations, incidence modeling, ANC or sentinel surveillance, integrated behavioral and biological surveys, drug resistance estimates.
- Other types of staff not covered by the above categories (e.g., data capturers, data clerks, security guards, cleaners, etc.).
Type of Support Provided by PEPFAR to the Staff: For each cadre category supported by PEPFAR at the site level and above site level (both service and non-service delivery) report the total amount spent for the workers across four categories.
- Salary: Total amount of salary support provided by PEPFAR, even if the health worker receives partial support from sources other than PEPFAR. PEPFAR salary support is any ongoing monetary contribution bench marked toward a total salary which is benchmarked toward, a government salary scale or international salary standard. A salary is characterized by being disbursed at regularly scheduled intervals in expected denominations.
- Stipend/Allowances: Total amount spent for each cadre on stipends and allowances. Stipends and allowances are separate from base salary. Stipend payments are not necessarily commensurate with, nor benchmarked toward, a government salary scale or international salary standard. These include one-time and supplementary payments, for example, for overtime worked due to HIV case burden, and financial benefits such as social security fund and health insurance. Payment could be made at regular intervals or intermittently depending on agreement.
- Non-monetary support only: Total amount spent on only non-monetary forms of support that do not involve currency, in connection with or in support of the provision of HIV services. These include mobile phone credits, general modes of transportation like bicycle or motorbike, job aids or equipment that can be used outside of HIV or in other jobs (such as in private practice), or other in-kind support. Include volunteers who work on HIV and receive only non-monetary support from PEPFAR.
This indicator is reported at the facility, community, and above-site levels.
Indicator changes (MER 2.0 v2.3 to v2.4): None
PEPFAR Support definition:
No additional requirements needed outside of the standard definition
Guiding narrative questions:
- For all categories of workers, including other, please provide description of specific cadres in the narrative.
- Please include descriptions of what type types of non-monetary support are captured (e.g., mobile phone credits, equipment, bicycles, etc.).
- Please confirm that workers listed as under non-monetary receiving only non-monetary support (not in addition to salary or stipend)?